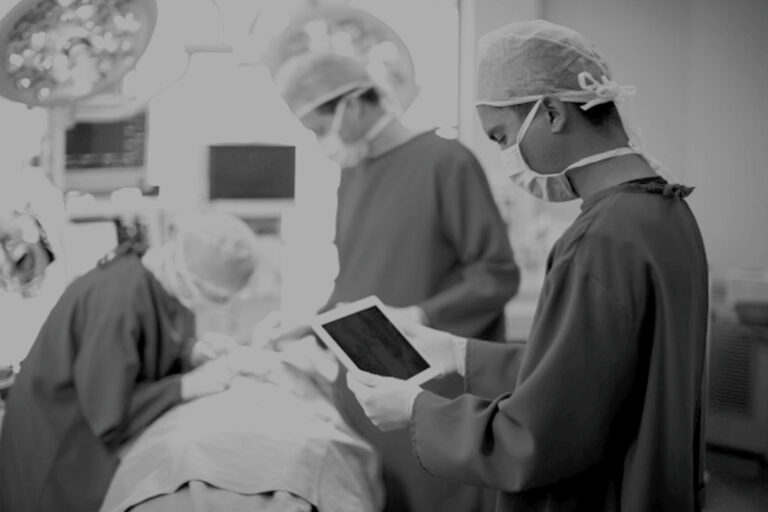
By Tracy Rausch, Chief Innovation Officer and Founder
In my work as a Clinical Systems Engineer in both the public and private healthcare sectors, I have witnessed the almost impossible situation Chief Nursing Officers (CNOs) find themselves in daily. On the one hand, they must maintain patient safety and improve treatment outcomes in ICUs that may exceed their optimal patient census. On the other hand, they need to contend with a shortage in the very resources they need to achieve this goal – their nursing staff. And as if these were not enough, CNOs also are tasked, as part of their management responsibilities, to do their part to help maintain financial ICU viability.
By juggling the solutions to these three challenges – patient wellbeing, staff nurse attrition and ICU finances – CNOs may also find themselves facing an unenviable Catch 22 since solving one problem may inadvertently exacerbate another. Increasing the number of patients per nurse, for example, will relieve some staffing pressures. but will increase burn-out. It also could negatively impact patient treatment outcomes, ICU patient safety, patient satisfaction and overall quality of care. And expanding hours and bringing in travel nurses, for example, may help better ensure patient quality of care, but may increase staff frustration and turnover while adding to a providers’ variable costs. Many CNOs often have no choice but to “rob Peter to pay Paul” and may end up not really making any of their constituents happy.
But in the current “do more with less” environment, CNOs must look beyond quick fixes and help to identify solutions for organization management that have the potential to solve these multiple – and oftentimes seemingly competing – challenges at the same time and over the longer term. From our extensive work and research at DocBox with ICU nurses, staff nurses and provider management, I believe that this can be achieved through three interrelated strategies:

The first is to address those factors that contribute to nurse burnout and attrition which can be most readily remedied over the short term and with minimal incremental expense. Recent research suggests that burnout is one of the reasons that millennial and Gen Z nurses will stay with their employing provider for approximately only two years before leaving. Compounding this problem, the U.S. Bureau of Statistics projects the need for over 1 million RNs over the next few years to help providers expand their nursing staffs and to replace those nurses that are retiring. Given this staggering number and expected high turnover with newer staff, anything a provider can do to improve nurses’ job satisfaction could be expected to increase retention and decrease attrition.
One identified stressor for nursing staff is the amount of time they need to dedicate to nonclinical tasks. These include charting, inputting data into a patient’s EHR, scheduling post-discharge follow-up, tracking medication and medical device usage, and patient advocacy activities. In addition to the time demands of these tasks, I can tell you from seeing how much admin work nurses need to do, that it also can distract and divert them away from why they became nurses in the first place, which is, of course, top notch patient care. EHR systems must be easy to learn with minimal time commitment for training; easy to remember how to use between uses, especially for part-time and travelling staff; easy to use; with efficient-minimal computer touches to accomplish tasks; and pleasant to use.
The second is to provide nursing staff, who are already doing superhero work, with the tools they most need to improve patient care in the ICU. Even with a 1:1 or a 1:2 nurse-to-patient ratio, the demands on a nurse’s time in providing patient care in an ICU are enormous. These nurses need to be able to monitor patients 24/7 and in real time to ensure their safety. They also need to interact with other members of the patient healthcare teams and must have quick and easy access to critical patient information in order to best represent patients with their team. This may be especially important for evidence-based practices (EBP) in nursing which involve having access to – and using – the best available information to improve patient treatment outcomes.
Nurses also need medical devices, including cutting edge IoMT applications, that have minimal downtime and require a minimal learning curve. The less time they spend learning how to use technology, the more time they will have to use it to help provide necessary critical care to their patients and the lower the cost of training. Less ramp-up time with life-saving technologies creates a win-win for everyone.
And in much the same way that helping nurses make the best and most efficient use of their time helps to reduce burnout and attrition, it also can contribute to more positive patient outcomes. It may also reduce such events as medication administration errors, missed nursing care episodes, infections, failure to rescue, and readmissions. Such omissions of care understandably also negatively impact job satisfaction (which then contributes to burnout and attrition, perpetuating the attrition cycle).
The third is making it easier for CNOs and their staff to help their colleagues on the revenue cycle team ensure that providers are reimbursed for all necessary expenses in the ICU while also taking steps to minimize waste (which can increase costs). Given the complexity and pace of an ICU, it should not be surprising that the challenge for nursing staff to capture all cost activities is immense. And with all the other demands on ICU nurses and their CNO, trying to input all procedures, medications and device usage can prove daunting to say nothing of time consuming. In fact, research indicates that nursing staff in the ICU complete an average of 400 mouse clicks per shift. Another study showed that more than a third of a nurse’s time during each shift was spent on documentation and more than 80 percent of that time was spent away from the patient’s bedside.
While tracking billable patient medications, medical procedures, medical device usage and various supplies is a necessary function of the ICU and other staff, it should not unnecessarily or arbitrarily increase their workloads (and stress levels). Providers should streamline and automate the process as much as possible to facilitate ICU revenue recovery rather than having it divert precious nursing time from patient care.
The Path Forward
There have been a good number of studies done – with an equal number of solutions posited – to address these three challenges faced daily by CNOs. They include such ideas as including nurses in policy decisions; setting up self-help or more formal peer support systems to help nurses better manage stress and burnout; offering counseling and other psychological/emotional support; partnering with nursing schools for recruitment and training; regulated nurse staffing levels; mandated nurse-to-patient ratios; involving nurses in scheduling; and expanded education and training.
While all these solutions would provide tangible benefits to any CNO or provider, they often fall short, since they focus more on individual challenges, such as time constraints, stress, or revenue capture, rather than on providing an integrated solution that addresses multiple challenges simultaneously.
Believing that such an integrated solution was not only possible but readily achievable, DocBox worked with CNOs, nurses, physicians, and the healthcare community to better understand their needs, especially in the ICU setting. We then used this information to develop DocBox®, The Clinician Assistant in Critical Care™. With it, gathering data automatically from connected medical devices and other health IT systems including values and waveforms and capturing procedures and observations make nursing documentation at the bedside of ICU patients easier and more efficient. This also provides administrators with actionable operational data that assist in resource planning and optimization of the revenue stream. This achieves the three biggest challenges that I mentioned above – reducing documentation time by up to 70 percent, giving nurses more time to be nurses and thereby reducing stress and burnout; providing nurses with the tools to improve ICU patient care; and improving revenue capture.